What Is Prior Authorization In Insurance? Process & Tips


What Is Prior Authorization In Insurance? Process & Tips
Every year, physicians spend an average of 13 hours per week dealing with prior authorization requests. For healthcare vendors building digital solutions, understanding what is prior authorization isn't just helpful, it's essential to creating tools that actually solve problems for health systems.
Prior authorization is the approval process insurance companies require before they'll cover certain medications, procedures, or services. It's meant to control costs and ensure medical necessity, but in practice, it often creates delays that frustrate patients, providers, and the vendors trying to serve them. Denied or delayed authorizations can mean postponed treatments, increased administrative burden, and strained relationships between payers and providers.
At VectorCare, we help healthcare vendors build SMART on FHIR applications that integrate directly into EPIC workflows, including those that streamline prior authorization processes. Whether you're developing clinical decision support tools, remote monitoring platforms, or care coordination solutions, knowing how prior authorization works will help you design products that reduce friction rather than add to it.
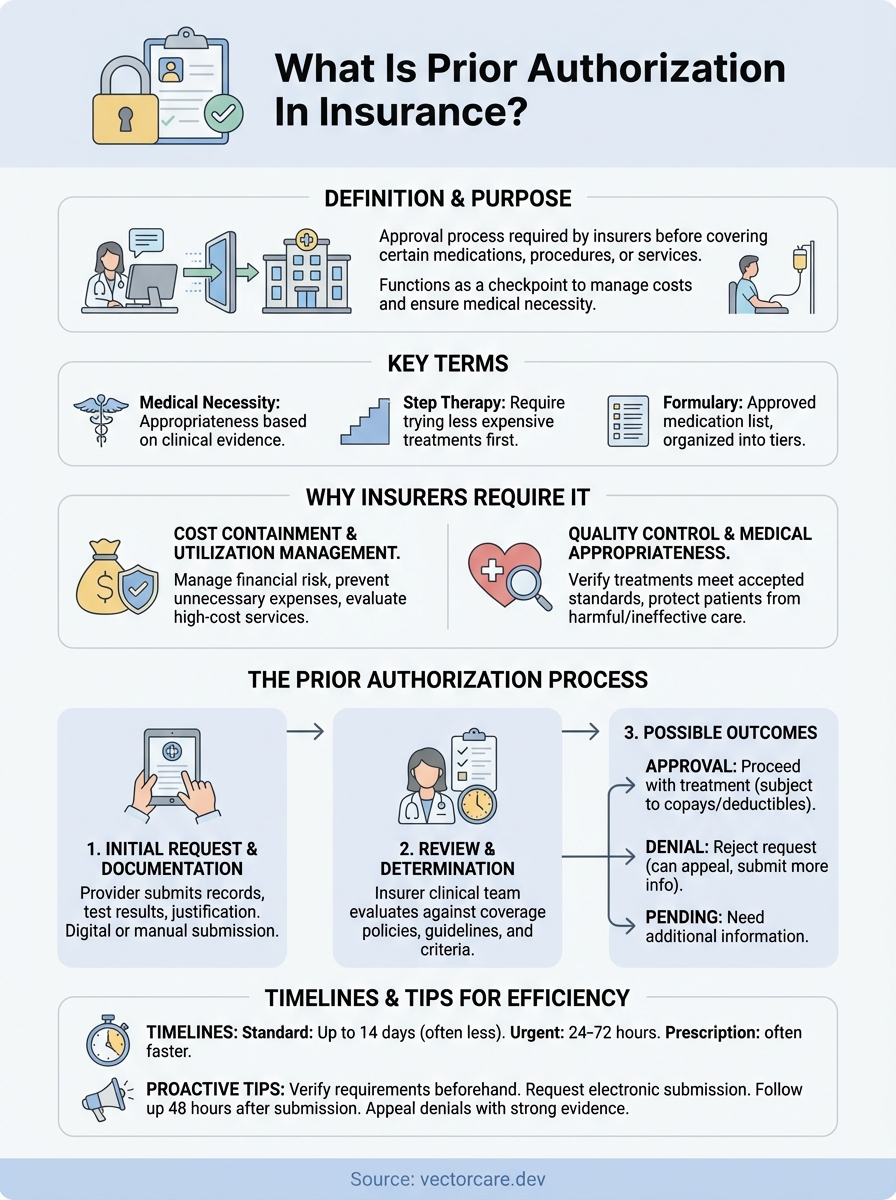
This guide breaks down the prior authorization process, explains why insurers require it, and offers practical tips for navigating it more efficiently.
Prior authorization meaning and key terms
When you're building healthcare technology, understanding what is prior authorization means going beyond a simple definition. Prior authorization (sometimes called precertification or preapproval) is the process where your healthcare provider requests approval from your insurance company before delivering specific medical services, prescriptions, or procedures. Insurance plans use this gate-keeping mechanism to verify that a proposed treatment meets their coverage criteria and medical necessity standards before they commit to paying for it.
The basic concept
Prior authorization works like a checkpoint in your care journey. Your doctor submits a request to your insurance company that includes medical records, diagnostic results, and justification for why you need a particular treatment. The insurer then reviews this information against their coverage policies and clinical guidelines to decide whether they'll pay for the service. This process can apply to expensive medications, advanced imaging like MRIs, specialty referrals, or surgeries that cost your insurance company significant money.
The system affects you directly because no authorization means no coverage. If your provider moves forward without getting approval first, you could face the full cost of treatment out of pocket. Insurance companies argue this protects against unnecessary care and keeps premiums lower, while providers often see it as administrative burden that delays patient care.
"Prior authorization acts as a financial and clinical review step between a provider's recommendation and an insurer's agreement to pay for that care."
Essential terminology you'll encounter
You'll run into specific terms when dealing with prior authorization that have precise meanings in the insurance world. Medical necessity refers to the standard insurers use to determine if a treatment is appropriate and required for your condition based on clinical evidence. Your insurance company won't approve services they consider experimental, cosmetic, or outside accepted medical practice, even if your doctor recommends them.
Step therapy (or fail-first protocols) requires you to try less expensive treatments before your insurer will approve costlier alternatives. For example, you might need to try three generic medications before getting approval for a brand-name drug. Formulary describes your insurance plan's approved medication list, typically organized into tiers that affect your copay amounts. Denial means your insurer rejected the authorization request, though you can usually appeal this decision through a formal process. Understanding these terms helps you navigate conversations with both your provider's office and your insurance company when authorization issues arise.
Why insurers require prior authorization
Insurance companies implement prior authorization requirements primarily to manage their financial risk and control healthcare spending. When you understand what is prior authorization from the insurer's perspective, you see it functions as their tool to prevent unnecessary medical expenses before they occur. Health plans use this approval process to verify that proposed treatments align with evidence-based guidelines and that less expensive alternatives have been considered first. Without this checkpoint, insurers argue they would face billions in potentially avoidable costs from procedures that might not meet medical necessity standards or could be replaced with more cost-effective options.
Cost containment and utilization management
Your insurance company evaluates high-cost services through prior authorization to avoid paying for treatments that might not provide sufficient clinical benefit relative to their price. Specialty medications can cost tens of thousands of dollars annually, and advanced procedures like certain surgeries or imaging studies carry price tags that significantly impact your plan's overall spending. Insurers require authorization for these expensive items to ensure they're medically appropriate before committing to payment. This process also catches instances where providers might order duplicate tests or prescribe brand-name drugs when equally effective generics exist at a fraction of the cost.
"Prior authorization serves as the insurance industry's primary mechanism to control healthcare utilization and spending before services are delivered."
Quality control and medical appropriateness
Beyond cost concerns, your insurer uses prior authorization to verify that proposed treatments meet accepted standards of care for your specific condition. Insurance companies employ clinical teams, often including physicians and pharmacists, who review authorization requests against medical literature and professional guidelines. They look for situations where a treatment might carry unnecessary risks, lack supporting evidence, or fall outside established protocols for your diagnosis. This review process aims to protect you from potentially harmful or ineffective care, though providers often view it as interference with their clinical judgment.
How the prior authorization process works
Understanding what is prior authorization means knowing the step-by-step workflow that connects your provider's office to your insurance company's approval system. The process typically begins when your doctor identifies that a proposed treatment, medication, or procedure requires authorization based on your insurance plan's requirements. Your provider's staff then initiates a formal request that triggers a series of reviews and communications between the healthcare facility and your insurer. This workflow can happen through phone calls, fax submissions, or electronic portals, with most health systems now moving toward digital submission methods that integrate directly with insurance company systems.

Initial request and documentation
Your provider's administrative team gathers the necessary information to submit your authorization request to your insurance company. They collect your medical records, diagnostic test results, treatment history, and clinical notes that justify why you need the specific service or medication. The staff completes your insurer's required forms, which ask for diagnosis codes, procedure codes, expected treatment dates, and detailed explanations of medical necessity. Your provider must demonstrate that the proposed treatment meets your insurance plan's coverage criteria and follows accepted clinical guidelines for your condition. This documentation package gets submitted through your insurer's preferred channel, whether that's an online portal, phone-based system, or direct electronic integration with the insurer's authorization platform.
Review and determination
Your insurance company assigns your authorization request to a review team that evaluates the submitted information against their coverage policies. Clinical reviewers, often nurses or pharmacists, examine whether your proposed treatment aligns with evidence-based guidelines and their plan's specific requirements. They check if you've tried required step-therapy medications first, verify that the provider is in-network, and confirm the service meets medical necessity standards for your diagnosis. The reviewer can approve the request immediately, request additional documentation from your provider, or escalate complex cases to a physician reviewer for further evaluation.
"The authorization workflow moves through distinct stages of submission, clinical review, and determination that directly impact when you can receive approved care."
Timelines, decisions, and exceptions
Knowing what to expect after your authorization request goes in helps you plan your care and understand your options if things don't move as quickly as you need. Insurance companies operate under specific timeframes dictated by state and federal regulations, though actual processing times vary based on the urgency of your situation and the complexity of your case. Your provider's staff tracks these requests, but you should also monitor the status through your insurer's member portal or by contacting them directly to avoid unexpected delays in starting treatment.

Standard decision timeframes
Your insurance company must respond to non-urgent authorization requests within 14 days under federal guidelines, though many states impose shorter deadlines of 72 hours or less. Urgent requests that your doctor marks as requiring immediate medical attention typically get responses within 24 to 72 hours. Your insurer counts business days from when they receive complete documentation, so missing information restarts this clock. Prescription prior authorizations often process faster than procedure requests, with many getting decisions within 24 to 48 hours through automated electronic systems that connect pharmacies directly to insurance company databases.
Possible outcomes and what they mean
Your authorization request receives one of three decisions from your insurance company. An approval means you can proceed with the treatment at the coverage level your plan specifies, though you'll still pay your normal copays or deductibles. A denial requires your provider to either submit additional documentation, appeal the decision, or help you explore alternative treatments your plan will cover. Pending status means your insurer needs more information before making a decision, which extends your waiting period until they get what they need.
"Authorization decisions directly impact when you can start treatment and how much you'll pay out of pocket for approved services."
Emergency situations and expedited processing
You can request expedited review when your doctor certifies that waiting through standard timelines could seriously harm your health or ability to function. Insurance companies must respond to these urgent requests within 72 hours, and many states require decisions within 24 hours for true emergencies.
How to avoid delays and handle denials
You can take specific actions to move authorization requests through the system faster and increase your approval chances. Understanding what is prior authorization from a practical standpoint means knowing how to work within the system rather than against it. Your provider's office handles most authorization logistics, but staying informed and proactive about your case helps catch problems early. Missing documentation and incomplete submissions cause the majority of delays, so confirming your provider has everything they need before submission saves you valuable time.
Proactive steps to prevent delays
Call your insurance company before your doctor submits the authorization request to verify exactly what documentation they require for your specific treatment. Ask your insurer's prior authorization department for their clinical criteria, required test results, and any step-therapy requirements you must complete first. Provide your provider's office with your insurance card, current plan details, and any previous authorization numbers for related treatments. Request electronic submission when possible since digital requests typically process faster than fax or phone submissions. Follow up with both your provider and insurer 48 hours after submission to confirm receipt and check for any missing information they need to complete their review.
"Proactive communication with both your provider's authorization team and your insurance company prevents most delays before they happen."
When to appeal a denial
File an appeal immediately if your insurer denies your authorization request and your doctor still believes the treatment is medically necessary. Your insurance company must provide written explanation for denials that includes specific reasons and your appeal rights. Ask your provider to submit additional clinical documentation, peer-reviewed studies, or expert opinions that support your case. Most insurers offer multiple appeal levels, starting with internal reviews and potentially escalating to external independent review organizations if your state allows it.
Wrap up and what to do next
Understanding what is prior authorization gives you the foundation to build healthcare technology that actually reduces administrative burden for providers and patients. Prior authorization remains one of the biggest pain points in healthcare workflows, creating delays that affect patient care and strain provider resources. Your awareness of the process, timelines, and common denial reasons positions you to design solutions that address these friction points directly.
Take action by examining how your product interacts with authorization workflows in EPIC and other EHR systems. If you're building tools for healthcare vendors, consider how integrating authorization status checks, documentation support, or automated submissions could differentiate your solution in the market. VectorCare helps healthcare companies build and deploy SMART on FHIR applications that embed directly into clinical workflows, including those that streamline prior authorization processes. When you reduce the time physicians spend on administrative tasks, you create real value that health systems will pay for.
The Future of Patient Logistics
Exploring the future of all things related to patient logistics, technology and how AI is going to re-shape the way we deliver care.