Data Provenance vs Data Lineage: Differences In Governance


Data Provenance vs Data Lineage: Differences In Governance
Healthcare vendors working with EHR integrations handle sensitive patient information that flows through multiple systems, APIs, and workflows. When a compliance auditor asks where a specific data point originated or how it reached its current state, vague answers don't cut it. Understanding data provenance vs data lineage becomes essential, not just for passing audits, but for building trustworthy integrations that health systems actually want to deploy.
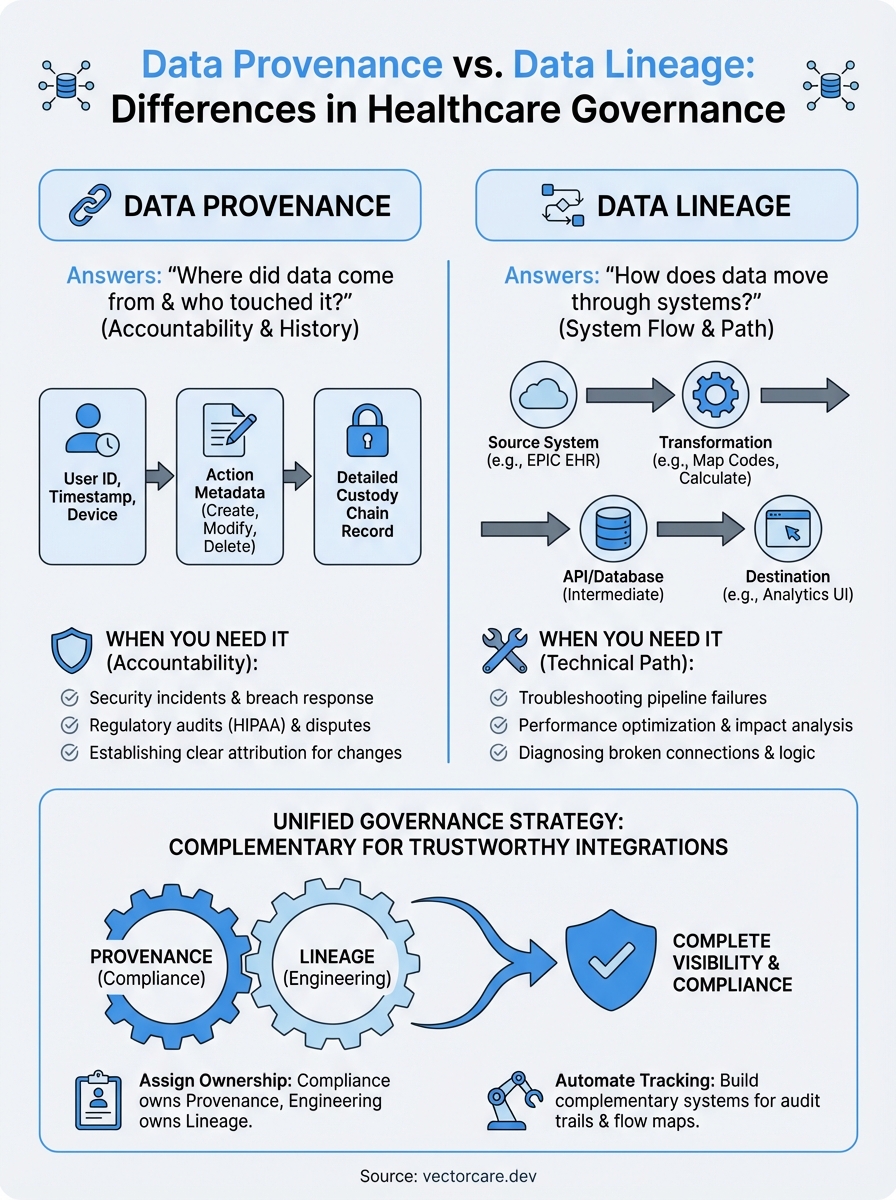
These two terms often get used interchangeably, which creates confusion during governance discussions and technical planning. Data provenance answers "where did this data come from and who touched it?" while data lineage answers "how does data move through our systems?" Both matter, but they serve distinct purposes in your data governance strategy. Getting them mixed up can lead to gaps in compliance documentation or inefficient troubleshooting when something breaks.
For healthcare vendors building SMART on FHIR applications, especially those integrating with EPIC systems through platforms like VectorCare, grasping these differences directly impacts how you design workflows and maintain HIPAA compliance. This article breaks down what separates data provenance from data lineage, explores their specific use cases in healthcare contexts, and explains how they work together within a comprehensive governance framework.
Why provenance and lineage matter in healthcare data
Healthcare organizations deal with protected health information (PHI) that flows through dozens of systems, transformations, and human touchpoints before it reaches a clinician's screen. When a medication dosage appears in a patient chart, that single value carries enormous weight because prescribers trust it to be accurate, current, and sourced correctly. Your ability to trace that data's journey from its origin through every transformation determines whether that trust is justified or dangerously misplaced.
Compliance audits demand complete documentation
HIPAA enforcement doesn't accept hand-waving about data handling practices. When your organization faces an audit or responds to a breach disclosure, auditors expect detailed records showing exactly who accessed what data and how that information moved between systems. You need to demonstrate not just that security controls exist, but that you can reconstruct the complete chain of custody for any patient record, down to specific timestamps and user actions.
The difference between passing and failing these audits often comes down to how thoroughly you've documented your data flows. State health departments, OCR investigators, and internal compliance teams all require evidence that your systems maintain proper access controls and audit trails. Missing documentation creates legal exposure that most healthcare vendors can't afford, especially when competing for contracts with risk-averse health systems.
Without clear records of data origins and transformations, you're asking regulators to trust your word rather than your evidence.
Clinical workflows break when data lacks context
A referring physician sends a patient to a specialist with test results that appear incomplete or contradictory. The specialist spends 15 minutes trying to figure out which lab ran the tests and whether the units match their internal standards. This scenario repeats thousands of times daily in integrated delivery networks, burning clinical time and introducing potential diagnostic errors that compromise patient safety.
Your SMART on FHIR application might pull glucose readings from multiple sources like continuous monitors, lab draws, and manual entries. When those values conflict, clinicians need immediate clarity about which source takes priority and how recent each reading actually is. Understanding data provenance vs data lineage becomes directly tied to clinical decision quality because the wrong prioritization can lead to incorrect insulin dosing or missed hypoglycemic episodes.
System failures need rapid root cause analysis
When your integration suddenly starts pushing blank values into critical fields, your engineering team can't waste hours manually tracing through logs. You need automated lineage tracking that shows exactly where the pipeline broke and which upstream changes triggered the failure. Health systems evaluating your application expect proof that you can diagnose and fix data issues faster than their current workflows allow.
Production incidents in healthcare settings carry higher stakes than typical SaaS failures. A broken referral workflow doesn't just frustrate users, it delays patient access to specialty care and potentially worsens health outcomes. Your ability to quickly identify whether the issue stems from FHIR resource mapping errors, authentication failures, or upstream EHR changes determines how long that degraded service persists.
What data provenance is and what it records
Data provenance creates a historical record of every action performed on a specific piece of data from its initial creation through all subsequent modifications. Think of it as a detailed custody chain that documents who created the data, when they created it, which systems or processes transformed it, and what changes occurred at each step. In healthcare contexts, provenance answers accountability questions that compliance officers and clinical staff actually need answered when investigating data quality issues or security incidents.
The metadata provenance captures
Provenance systems record metadata about data rather than the data values themselves. When a nurse enters a patient's blood pressure reading into an EHR, provenance tracks the nurse's user ID, timestamp, device or workstation identifier, and the specific FHIR resource that stored that measurement. You capture authentication details showing which credentials authorized the write operation and whether the action went through an API integration or direct user input.

This metadata extends beyond simple creation events. Provenance logs track every modification, deletion, or access event that touches a data element. When your SMART on FHIR application updates a patient's medication list, the provenance record shows your application's identity, the specific API call used, the original values before your update, and the new values after transformation. Health systems reviewing your integration can verify that your application maintains proper attribution for all changes it introduces into their production EHR.
Why custody chains matter for vendors
Understanding data provenance vs data lineage becomes critical when you face questions about data integrity and regulatory compliance. If a health system discovers that incorrect demographic information caused a medication to be sent to the wrong pharmacy, provenance records let you trace back to see whether your integration introduced the error or simply passed along corrupted data from an upstream source. You avoid taking blame for issues outside your control when you can demonstrate clear custody of every transformation your code performs.
Provenance documentation protects your vendor relationship by proving exactly which system caused data quality problems.
Your HIPAA Business Associate Agreement requires you to produce audit trails showing who accessed PHI and what they did with it. Provenance records fulfill this requirement by logging every read, write, and modification event that flows through your integration. State breach notification laws often mandate these same records when determining whether an incident qualifies as a reportable breach.
What data lineage is and what it maps
Data lineage tracks the complete path data takes through your systems from its source to its final destination, documenting every transformation, calculation, and routing decision along the way. Instead of focusing on who touched the data like provenance does, lineage shows how data moves between applications, databases, APIs, and processes. When you build a SMART on FHIR integration that pulls patient demographics from EPIC, transforms them into a standardized format, enriches them with external data, and pushes results to an analytics platform, lineage maps that entire journey as a technical workflow.
How lineage maps system-to-system flows
Your lineage documentation shows which systems feed data to which downstream consumers and the exact sequence those transfers follow. When a patient's medication list starts in EPIC's FHIR server, gets pulled into your application through a MedicationRequest query, flows through your business logic layer, and then gets written to an external pharmacy system, lineage tracks each hop in that chain. You document API endpoints, database tables, transformation functions, and integration points that participate in the flow.
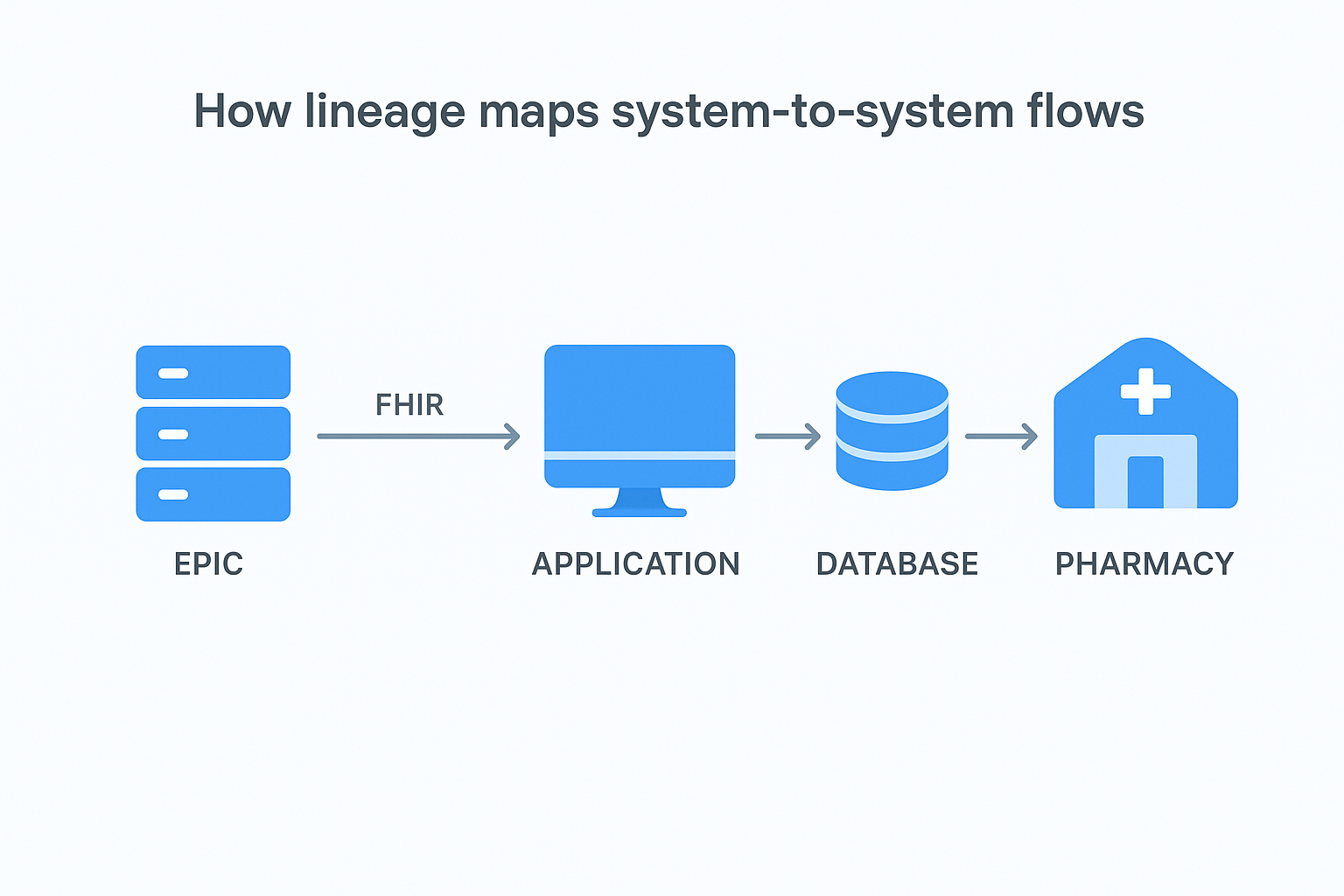
This mapping becomes essential when troubleshooting integration failures. If medication orders suddenly stop reaching pharmacies, your lineage documentation lets you pinpoint which connection broke without manually checking every system. Health systems evaluating your application want proof that you understand your own data flows well enough to diagnose problems quickly, and comprehensive lineage charts demonstrate that operational maturity.
Lineage documentation turns opaque data pipelines into transparent workflows that engineering teams can actually debug.
What transformations lineage documents
Lineage records capture every business rule, calculation, or format conversion your application performs on data as it moves through your integration. When you convert FHIR observation values from one unit system to another, map EPIC's medication codes to RxNorm identifiers, or aggregate multiple patient encounters into summary statistics, those transformations appear in your lineage documentation. You track input schemas, output schemas, and the specific logic that bridges them.
Understanding data provenance vs data lineage clarifies why you need both for complete governance. Lineage shows that your application transforms glucose readings from mg/dL to mmol/L at a specific pipeline stage, while provenance records which user or system initiated that conversion and when it occurred. The technical flow diagram comes from lineage, while the accountability trail comes from provenance.
Data provenance vs data lineage in practice
Your integration pulls patient allergy information from EPIC and displays it in a referral workflow. When a clinician questions whether the displayed sulfa allergy is current, you face two different investigative paths depending on whether you need provenance or lineage information. Provenance tells you that Dr. Sarah Chen updated that allergy record on February 15, 2026 at 14:32 UTC using workstation ID WS-4429, while lineage shows that the allergy data flowed from EPIC's AllergyIntolerance resource through your FHIR query layer, into your cache database, and finally to your React UI component. Both answers matter, but they solve fundamentally different problems.
When you need provenance answers
Security incidents and data quality investigations demand provenance documentation because you need to establish accountability for specific actions. When your health system partner reports that a patient's home address changed unexpectedly in their system, your provenance logs show whether your integration made that update or whether you simply read and displayed data that another system had already modified. You track the specific API call, authenticated user, and timestamp that triggered the change, which protects your vendor reputation when errors originate elsewhere.
Provenance answers the accountability question that determines whether your engineering team needs to fix a bug or whether you need to escalate to another vendor.
Clinical documentation disputes also require provenance records. If a nurse claims she entered a blood pressure reading that never appeared in the patient chart, your provenance logs either confirm her entry with a timestamp or demonstrate that no write operation occurred from her credentials during that shift. These records become evidence in medical malpractice cases and compliance investigations where finger-pointing wastes time unless you can produce definitive proof.
When you need lineage answers
Pipeline failures and performance optimization projects require lineage documentation because you need to understand system-to-system flows rather than individual actions. When your medication reconciliation feature suddenly takes 45 seconds instead of 3 seconds to load, lineage mapping shows you that the slowdown happens during the transformation step where you normalize drug codes, not during the initial FHIR query. You identify the exact pipeline stage causing problems without instrumenting every component manually.
How to use both in data governance
Your data governance framework needs both provenance and lineage tracking working together because they address different compliance and operational requirements. Healthcare vendors building EPIC integrations face audits that demand accountability records while simultaneously needing technical documentation that helps engineering teams maintain reliable pipelines. You implement provenance systems to satisfy regulatory audit trails and lineage mapping to support troubleshooting and impact analysis when you modify existing workflows or add new integration points.
Build complementary documentation systems
Your provenance implementation captures every data access, modification, and deletion event with metadata about who performed the action and when it occurred. You configure your FHIR integration layer to log authenticated user IDs, API credentials, timestamps, and the specific resources accessed during each transaction. These logs feed into your audit database where compliance officers can query historical actions without bothering your engineering team for manual log reviews.
Lineage documentation takes a different form because it maps system architectures rather than individual events. You maintain technical diagrams showing how data flows from EPIC's FHIR endpoints through your application components and into downstream systems. Your lineage records include transformation logic, business rules applied at each stage, and dependencies between different pipeline components. When you update a medication mapping function, your lineage documentation shows which downstream reports and workflows depend on that transformation.
Treating data provenance vs data lineage as competing approaches misses the point that governance requires both perspectives for complete visibility.
Assign ownership across teams
Your compliance team owns provenance record retention and audit response because they handle regulatory inquiries and breach investigations. They define retention policies that meet HIPAA's six-year requirement and configure alerting rules that flag suspicious access patterns or unauthorized data exports. You give them read-only access to provenance logs without requiring them to understand your technical architecture.
Engineering teams own lineage documentation and maintenance because they design data pipelines and troubleshoot integration failures. They update lineage diagrams when deploying new features and use those maps to conduct impact analysis before making schema changes or retiring legacy systems.
Automate tracking where possible
Your SMART on FHIR platform should generate provenance records automatically whenever your application reads or writes FHIR resources. You instrument your API layer to capture request metadata without requiring developers to add manual logging statements. Many healthcare integration platforms include built-in provenance tracking that creates audit trails compliant with FHIR's Provenance resource specification.
Lineage automation requires data catalog tools that scan your codebase, database schemas, and API configurations to generate flow diagrams. You connect these tools to your CI/CD pipeline so lineage documentation updates automatically when engineers deploy code changes that modify data transformations or add new integration endpoints.
What to do next
Your healthcare integration needs both provenance and lineage tracking working together to satisfy compliance requirements and maintain operational reliability. You can't choose between them because auditors demand accountability records while your engineering team needs technical documentation for troubleshooting complex workflows. Understanding data provenance vs data lineage helps you design SMART on FHIR applications that health systems actually trust to handle sensitive patient data.
Building these governance capabilities from scratch adds months to your development timeline and requires specialized expertise in FHIR standards, HIPAA compliance, and EHR integration patterns. Most healthcare vendors lack the internal resources to implement comprehensive tracking systems while simultaneously building their core product features and competing for health system contracts.
VectorCare's no-code platform handles the technical complexities of EPIC integration including built-in provenance logging and automated lineage documentation for your SMART on FHIR applications. You get HIPAA-compliant audit trails and system flow mapping without writing custom tracking code, letting your team focus on solving clinical problems instead of building governance infrastructure from the ground up.
The Future of Patient Logistics
Exploring the future of all things related to patient logistics, technology and how AI is going to re-shape the way we deliver care.